In today’s healthcare environment, patient safety isn’t limited to skilled diagnostics or prompt treatment—it’s equally tied to a facility’s ability to maintain the highest standards of hygiene. Every detail counts, especially those that are easily overlooked. Discharge curtains—used every day, touched constantly, and rarely prioritized—are one such detail. When facilities skip regular servicing of these seemingly minor components, they expose themselves to serious hygiene risks that can ripple through entire departments.
This blog dives deep into the unseen dangers of neglected curtain care, the implications for infection control, and the importance of establishing a reliable discharge curtain service routine.
Why Discharge Curtains Matter More Than You Realize
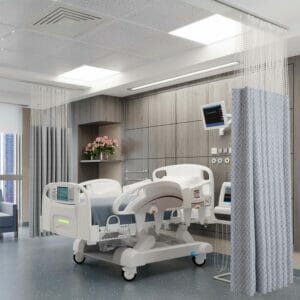
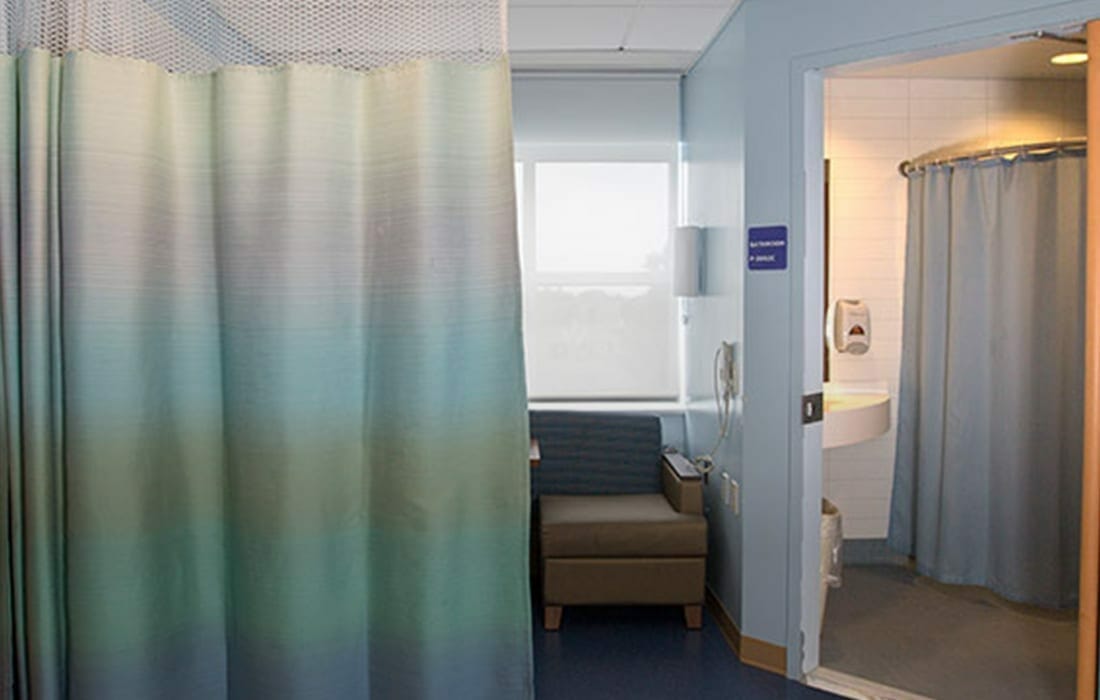
Discharge curtains are more than mere privacy barriers. Positioned in patient rooms, emergency bays, and examination areas, they are part of a hospital’s fabric—literally and metaphorically. Yet their purpose extends beyond aesthetics or patient dignity. These curtains often serve as the first line of separation between infected and vulnerable individuals, making them a frontline player in disease prevention.
However, their very function—being present in high-touch, high-traffic environments—makes them susceptible to contamination. Healthcare staff frequently touch these curtains while caring for patients, often without washing their hands before or after. Multiply this across hundreds of interactions daily, and the curtain becomes a silent host for bacteria, viruses, and spores.
Pathogen Build-Up: A Silent and Serious Threat
Studies show that soft surfaces like curtains are capable of harboring pathogens for extended periods. Microorganisms such as MRSA (Methicillin-resistant Staphylococcus aureus), VRE (Vancomycin-resistant Enterococci), and even C. difficile can cling to curtain fibers for days or weeks. And because fabric is more difficult to disinfect thoroughly than hard surfaces, it often remains an unchecked source of microbial transmission.
Unlike countertops, bed rails, or medical tools, curtains are not always included in routine sanitization protocols. Some facilities may change them quarterly—or worse, only when visibly soiled. The result is a ticking hygiene time bomb: an object assumed to be clean simply because it’s always there.

The Hidden Impact on Patient Safety
Infection control is one of the cornerstones of patient safety. When facilities overlook curtain maintenance, they unwittingly compromise their infection prevention strategies. Every missed servicing is an opportunity for pathogens to transfer from one patient environment to another.
Imagine a scenario where a patient recovering from surgery is placed in a room where the discharge curtain was last cleaned six months ago. Even if the room was otherwise spotless, the curtain could still carry contaminants from the previous occupant. In the absence of visible stains or odors, the risk often goes undetected—until an infection occurs.
Hospital-acquired infections (HAIs) cost facilities billions annually, not to mention the human cost in suffering and extended stays. Preventing HAIs requires a comprehensive approach, and discharge curtain servicing must be part of that conversation.
Operational Setbacks from Neglected Curtain Maintenance
Beyond the clear hygiene implications, neglecting curtain servicing can also hinder operational efficiency. Dirty or damaged curtains must be replaced urgently, leading to unplanned downtimes or room closures. This results in logistical challenges, delays in patient transfers, and increased strain on cleaning staff.
Worse yet, non-compliance with hygiene regulations or failing audits can lead to reputational damage, penalties, and reduced patient trust. Healthcare administrators and facility managers must realize that curtain care is not optional—it’s part of an effective, scalable infection control program.
As discussed in this detailed guide on why a reliable discharge curtain service is essential for hospital efficiency, regular servicing can directly contribute to smoother operations and better patient outcomes.
The Lifecycle of a Clean Curtain: What “Regular” Really Means
So what qualifies as regular curtain servicing? Unfortunately, there’s no universal timeline that applies to all facilities. The answer depends on the environment, curtain material, patient turnover rate, and local infection control policies. That said, industry best practices suggest high-touch curtains be cleaned or replaced at least every 30 to 90 days.
Emergency departments and isolation rooms may require more frequent changes. Likewise, if a room is used to house an infectious patient, all soft surfaces—including curtains—should be changed before another patient is admitted.
A professional discharge curtain service ensures this process is consistent, efficient, and compliant. For hospitals aiming to implement reliable systems, the key is to adopt proactive rather than reactive practices.
You can learn more about how HAIGuard™’s discharge curtain service supports hospitals in meeting their hygiene protocols and scheduling needs without interrupting workflows.
Fabric Type Matters—More Than You Might Expect
Not all curtains are created equal. The type of fabric used plays a major role in its antimicrobial properties, durability, and ease of cleaning. Some materials naturally resist moisture and bacterial colonization, while others absorb contaminants and are harder to sanitize effectively.
Incorporating high-performance fabric into your cubicle curtain system isn’t just a design choice—it’s a hygiene decision. Facilities that invest in quality fabric options reduce the frequency of needed replacements and improve long-term patient safety.
For a deeper dive into how material selection affects curtain performance, explore this resource on the role of fabric choice in custom cubicle curtains.
Staff Habits Can Undermine the Cleanliness Cycle
Even if curtains are cleaned on a proper schedule, improper staff handling can shorten the lifespan of that cleanliness. When healthcare providers touch curtains without gloves, or worse, after contact with patients or contaminated surfaces, the transmission of germs becomes almost inevitable.
That’s why any discharge curtain hygiene protocol must go hand-in-hand with staff education. Hand hygiene awareness and standard operating procedures for curtain handling should be incorporated into onboarding, infection control training, and daily routines.
Proper use of personal protective equipment (PPE) and signage reminding staff of touchpoints can reinforce this practice without disrupting workflows.
Regulatory Guidelines and Industry Expectations
While curtain hygiene might not always be top of mind, regulatory bodies have taken increasing interest in soft surface sanitation. Healthcare accreditation agencies often include curtain maintenance in their hygiene audits. OSHA and CDC guidelines both emphasize minimizing cross-contamination risks through environmental cleanliness.
Institutions that fail to meet these expectations risk more than fines—they risk legal liability, reputational harm, and declining patient confidence. In an era of patient reviews and digital transparency, perceived negligence—even in something as simple as curtain care—can influence public perception and trust.
Keeping a documented curtain servicing schedule and aligning with a certified provider adds accountability to your infection control framework.
Building a Sustainable Curtain Hygiene Strategy
Achieving consistent cleanliness requires more than occasional laundering. Hospitals and clinics must build a sustainable discharge curtain hygiene strategy that includes:
Inventory management: Maintaining a rotation stock of clean curtains to enable swift replacements.
Scheduling: Automating change-outs based on patient discharge, infection risk, or routine intervals.
Tracking systems: Using barcodes or RFID tags to monitor cleaning history.
Professional servicing partners: Partnering with specialists who understand healthcare compliance, turnaround times, and fabric performance.
It’s not enough to clean curtains reactively. A comprehensive plan—managed with the right tools and support—can transform curtain maintenance from an afterthought into a competitive advantage.
Beyond Cleanliness: Enhancing Patient Experience
A clean environment does more than reduce infection—it also improves patient perception. Clean, fresh curtains signal professionalism, attention to detail, and care for the patient experience. Patients and visitors may not always notice a spotless floor or a sanitized thermometer, but they’ll notice dingy or stained curtains.
Especially in sensitive settings like maternity wards, pediatric care units, or behavioral health facilities, environmental cues can deeply impact a patient’s sense of comfort and trust. Fresh, clean discharge curtains help create a more welcoming, reassuring space—one that communicates cleanliness on both a visual and psychological level.
Curtain Hygiene is Everyone’s Responsibility
It’s tempting to think of discharge curtains as static elements—just fabric hung between beds or around exam areas. But in reality, they are dynamic components of your infection prevention system. Every missed servicing creates an opening for bacteria to thrive, patients to fall ill, and reputations to suffer.
Regular, strategic curtain servicing isn’t just about cleanliness—it’s about compliance, efficiency, safety, and trust. Whether you manage a small clinic or a multi-wing hospital, integrating curtain hygiene into your broader cleaning protocols is a step toward a healthier future.
At HAIGuard™, we understand the impact clean environments have on patient outcomes and staff confidence. That’s why our discharge curtain services are designed to be consistent, hassle-free, and fully aligned with your facility’s infection control goals.
Don’t wait until issues arise. Make discharge curtain servicing part of your preventive strategy today.