In modern healthcare, infection prevention is not optional. As patient acuity rises and concerns over healthcare-acquired infections (HAIs) intensify, every surface, tool, and textile in clinical environments must withstand scrutiny. Among these, Hospital Curtains stand out as high-touch, frequently overlooked surfaces that can harbor pathogens and contribute to transmission risk.
At HAIGuard, we’ve always believed that effective infection control requires innovation, science, and real solutions tailored to the environments where care is delivered. In 2026, one of the most impactful advancements in environmental hygiene is the adoption of sporicidal treatments for hospital curtains — a shift that reflects both evidence-based practice and frontline clinical needs.
This comprehensive blog will explore the science behind sporicidal treatments, why they are now a standard for hospital curtains, how they integrate into broader infection prevention strategies, and what this means for patient safety, staff confidence, and healthcare quality outcomes.
1. Rethinking Hospital Curtains: From Aesthetic to Antimicrobial Priority
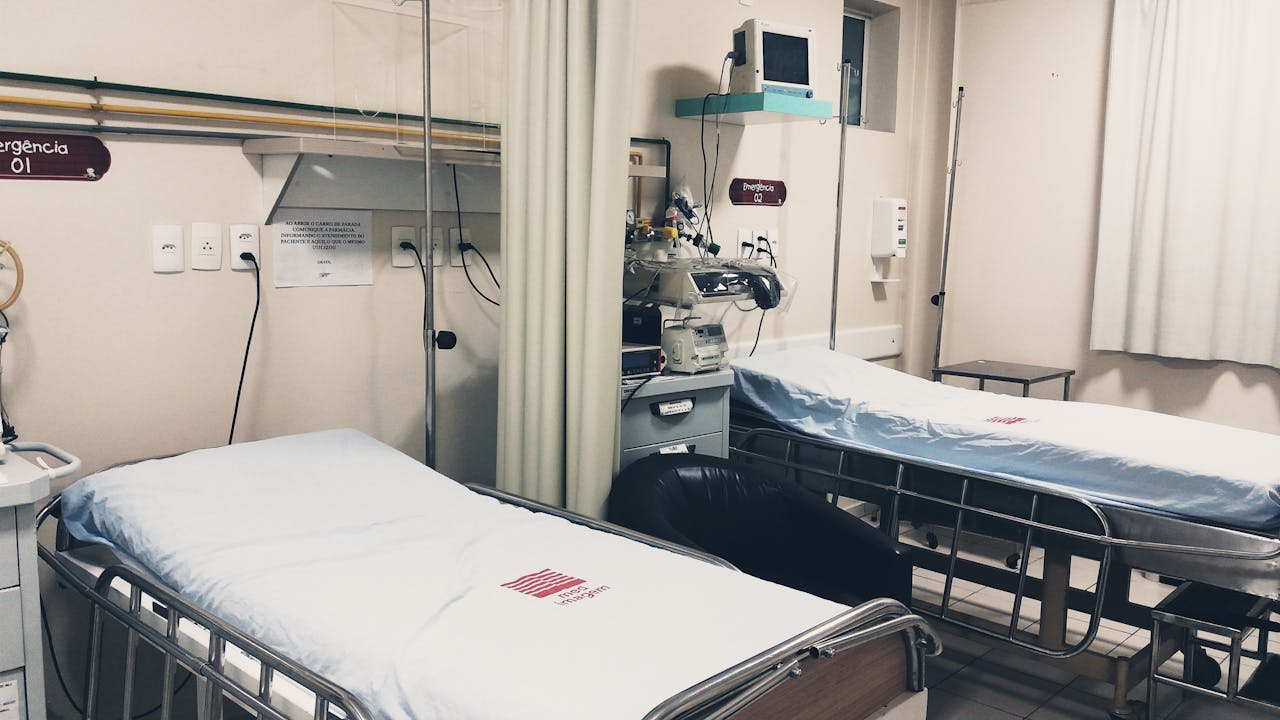
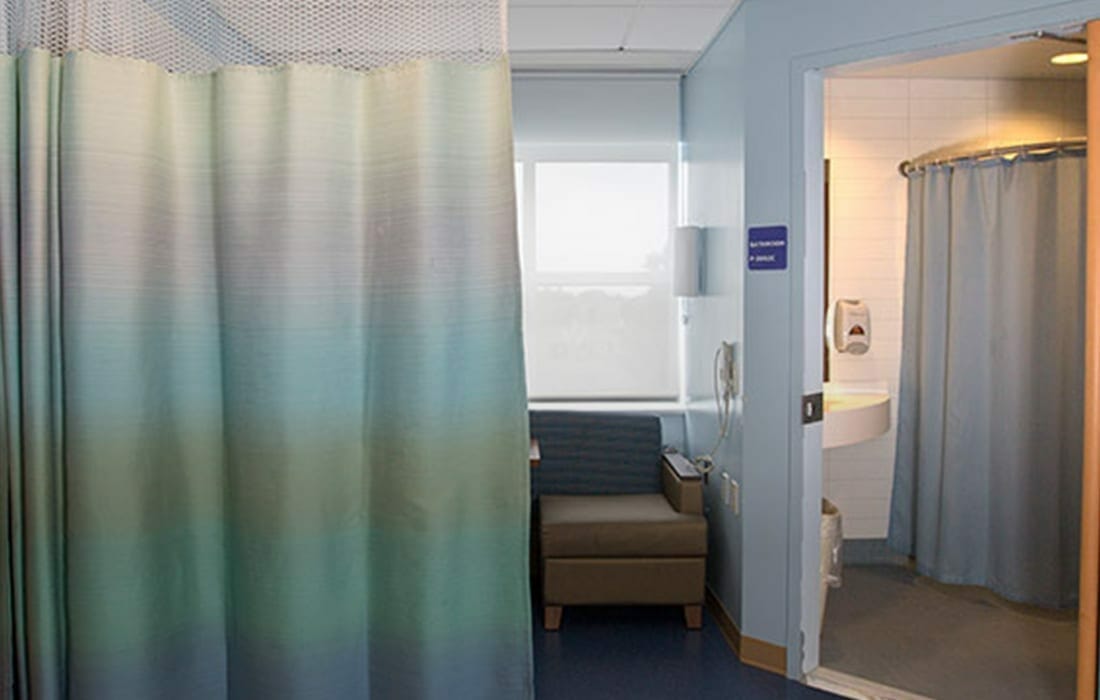
When most people think of hospital textiles, the focus is on bedding, gowns, and linens. Curtains, in contrast, are often seen as privacy tools rather than clinical surfaces. Yet in busy units — from intensive care to emergency departments — curtains are among the most frequently touched items.
Every adjustment for privacy, examination, or movement creates a point of contact. Consider a typical patient room: nurses touch the bed rails, monitors, and tubing, but they also pull, push, and reposition curtains repeatedly. Visitors, clinicians, and ancillary staff do the same. This high-contact nature transforms curtain fabric into a potential reservoir for pathogens.
Studies show that bacteria, spores, and viruses can persist on fabric surfaces for days or longer, surviving routine cleaning cycles and posing ongoing transmission risk. For pathogens like Clostridioides difficile, which form hardy spores, the risk is even greater. Ordinary detergents and disinfectants may reduce surface contamination, but they may not effectively eliminate spores.
That’s where sporicidal treatments come in — offering a new benchmark for textile hygiene, especially for Hospital Curtains.
2. Understanding Sporicidal Treatments
To appreciate why sporicidal technology is the new standard, we must first understand what it means.
2.1 What Are Spores and Why They Matter
Certain organisms — including C. difficile, some fungi, and resilient bacteria — produce spores. These microscopic, shielded forms are highly resistant to environmental stressors, including heat, dehydration, and many common disinfectants. Spores can persist on surfaces far longer than vegetative bacteria, posing prolonged risk.
In healthcare settings, spores are especially problematic. They can survive routine cleaning, transfer via contact, and resist conventional antimicrobial measures, leading to outbreaks and persistent contamination that standard protocols struggle to contain.
2.2 What Does “Sporicidal” Mean?
A sporicidal agent is one that can destroy spores — not just inhibit bacterial growth or reduce surface contamination temporarily. Sporicidal treatments disrupt the protective shell of spores, rendering them inactive and unable to germinate or transmit disease.
When applied to Hospital Curtains, sporicidal technology delivers a level of textile hygiene that traditional antimicrobial or disinfectant approaches cannot match.
**2.3 How Sporicidal Treatments Work on Curtains
Unlike sprays or surface wipes that act only momentarily, sporicidal treatments for curtains are integrated into the fabric or applied through validated industrial processes that provide sustained activity. This means:
- Persistent reduction of spore viability between routine launderings
- Enhanced defense against C. difficile and other spore-forming organisms
- Complementary protection alongside established infection control protocols
3. The Infection Prevention Imperative in 2026
Healthcare infection prevention programs have made tremendous strides over the past decade. Hand hygiene campaigns, medical device sterilization, surface disinfection, and antimicrobial stewardship have collectively reduced many infection types.
Yet HAIs remain a complex challenge. In 2026, facility executives and infection prevention leaders are holding themselves to higher standards than ever before. Reducing even a single HAI can translate into significant clinical and financial impact — fewer patient complications, shorter lengths of stay, lower readmission risk, and better quality scores.
Environmental hygiene is a critical pillar of this effort, and textiles like Hospital Curtains are increasingly understood to play a meaningful role in contamination pathways. In fact, many modern infection prevention protocols now include curtain assessment and hygiene as part of routine surveillance.
To better understand how the overall quality of curtains affects patient care and environment perception, read THE 2026 PATIENT EXPERIENCE: HOW HIGH-QUALITY PRIVACY CURTAINS MAKE A DIFFERENCE.
4. Standard Disinfection vs. Sporicidal Solutions: What the Evidence Says
Traditional environmental disinfection strategies — wipes, sprays, detergents — are essential. However, they have limitations when it comes to fabric surfaces and spore-forming organisms.
4.1 Limitations of Conventional Cleaning for Curtains
- Surface penetration challenges: Liquids may not fully penetrate curtain fibers.
- Transient effects: Most disinfectants act only at the moment of application.
- Resistance of spores: Many disinfectants do not inactivate hard-shell spores effectively.
- Frequency gaps: Curtains are not typically wiped multiple times per shift like hard surfaces.
These factors mean that between cleanings, curtains can repopulate with microbes — especially if they are in high-traffic areas.
4.2 The Advantage of Sporicidal Treatments
Sporicidal treatments provide a more robust safety layer:
- Demonstrated activity against spores
- Continuous surface protection between cleanings
- Reduction of persistent environmental reservoirs
- Support for infection surveillance efforts
This makes sporicidal standards especially relevant in areas where spore-forming pathogens are prevalent, such as gastrointestinal units, transplant wards, and long-term care sections.
5. Integrating Sporicidal Curtains Into Infection Control Programs
Effective infection prevention is holistic. No single product can prevent all HAIs. Instead, sporicidal curtains should be integrated into a broader strategy that includes:
- Rigorous hand hygiene compliance
- Routine surface disinfection
- Equipment sterilization protocols
- Patient cohorting and isolation practices
- Surveillance and data-driven performance monitoring
5.1 Collaboration Across Departments
Successful implementation requires cooperation between:
- Infection prevention teams
- Environmental services
- Nursing leadership
- Supply chain and procurement
- Facilities management
Each plays a role in ensuring that curtain hygiene is effective, measurable, and aligned with clinical workflows.
5.2 Tracking and Documentation
Incorporating curtain hygiene into quality dashboards and infection control metrics helps:
- Monitor contamination trends
- Correlate environmental hygiene with HAI outcomes
- Support accreditation and reporting requirements
Modern infection prevention programs increasingly view curtain hygiene as a KPI worth tracking.
6. Clinical Impact: Reducing HAI Risk Through Sporicidal Curtains
The ultimate goal of sporicidal treatments for Hospital Curtains is to reduce HAI risk. While individual outcomes vary based on unit type, patient mix, and existing protocols, research and real-world implementations point to measurable benefits.
6.1 Reducing Environmental Reservoirs
Studies indicate that environments with textiles treated for spore inactivation show:
- Lower surface counts of spore-forming organisms
- Reduced microbial burden over time
- Fewer instances of recontamination between cleanings
This translates into a safer care environment with fewer opportunities for indirect transmission.
6.2 Impact on Specific HAIs
Certain HAIs — especially those linked to C. difficile — are influenced by environmental contamination more than many clinicians once believed. Spores that persist on surfaces can easily touch hands, gloves, or equipment.
Sporicidal curtains help:
- Lower spore counts on high-contact fabric surfaces
- Support broader environmental decontamination efforts
- Interrupt transmission pathways that conventional disinfection might miss
7. Patient Confidence and Perception of Safety
In 2026, patients are more informed and more invested in their care environment than ever before. Visible cleanliness is no longer enough; patients and families seek reassurance that every precaution is taken to protect health and safety.
Investing in next-generation solutions like sporicidal hospital curtains communicates a commitment to:
- Cutting-edge infection prevention
- Evidence-based technology
- A safer healing environment
For patients who experience privacy with dignity and visible environmental quality, perception of care — and satisfaction scores — can improve in meaningful ways.
To explore how curtain quality influences patient experience, see BEYOND THE SURFACE: HOW ANTIMICROBIAL CURTAINS REDUCE HAI RATES IN 2026.
8. Operational and Economic Considerations
One of the most common concerns healthcare leaders face when evaluating new technologies is cost. When it comes to sporicidal hospital curtains, the conversation must focus on value over price.
8.1 Direct and Indirect Cost Benefits
Implementing sporicidal curtains may result in:
- Fewer infection-related interventions
- Reduced length of stay for affected patients
- Lower readmission rates due to infection complications
- Reduced environmental contamination cleanup workload
While the initial material cost may be higher than traditional curtains, the total cost of care — including prevented HAIs — often justifies the investment.
8.2 Operational Efficiency
Curtains treated with sporicidal processes can:
- Require fewer emergency changes
- Support consistent hygiene standards
- Integrate with existing laundry and replacement cycles
This reduces ad-hoc work for environmental services and supports predictable workflows.
8.3 Sustainability Considerations
Durability and extended lifecycle performance also contribute to sustainability. High-quality, sporicidally treated curtain fabrics often withstand repeated laundering and use, reducing waste and long-term procurement costs.
9. Choosing the Right Hospital Curtains for Your Facility
Not all curtain solutions are created equal. When evaluating options, healthcare facilities should consider:
- Verified sporicidal activity against relevant pathogens
- Compatibility with healthcare laundering processes
- Fire, safety, and compliance standards
- Durability and fabric performance
- Vendor support and warranty coverage
At HAIGuard, we design solutions that balance clinical performance, operational practicality, and long-term value.
10. Implementation Best Practices
Successfully adopting sporicidal hospital curtains requires thoughtful planning:
10.1 Conduct a Risk Assessment
Identify areas where spore-forming organisms are most likely to pose risk:
- Gastrointestinal care units
- Long-term acute care
- Rehabilitation areas
- High-traffic assessment zones
This ensures targeted deployment where impact is greatest.
10.2 Train Environmental Services and Clinical Staff
Clear protocols for:
- Curtain change procedures
- Laundering and handling
- Documentation and tracking
Training builds confidence, compliance, and consistency.
10.3 Monitor and Adjust Protocols
Collect data on:
- Curtain contamination counts
- HAI incidence trends
- Laundry turnaround times
- Staff feedback
Use this information to refine processes and demonstrate value.
11. The Future of Infection Prevention and Curtain Hygiene
Infection prevention is evolving rapidly. As pathogens adapt and patient populations shift, so must environmental controls. Spores were once viewed as nearly impossible to manage on fabrics like curtains. Today, sporicidal treatments have changed the paradigm.
Looking ahead, we anticipate:
- More real-time surface contamination monitoring
- Integration of textile performance into digital quality dashboards
- Broader adoption of evidence-based textile hygiene standards
- Greater alignment of infection prevention with sustainability goals
Hospital curtains will continue to be an essential element of this journey.
A New Standard of Clean for Hospital Curtains
The adoption of sporicidal treatments for Hospital Curtains is more than a trend. It reflects a deeper commitment to science, patient safety, and measurable quality outcomes.
By addressing one of the most overlooked vectors in clinical environments — fabric surfaces — healthcare organizations can strengthen infection prevention strategies, reduce risk, and support the broader goals of safer care delivery.
At HAIGuard, our mission is clear: to provide curtain solutions that meet the highest standards of cleanliness, performance, and clinical relevance. Sporicidal treatments represent the new standard — one that aligns with evidence, supports outcomes, and elevates patient and staff confidence.
If your facility is ready to adopt the next generation of clean for hospital curtains, we’re here to partner with you every step of the way.